Archistruction® is a disruptive force in the real estate industry that provides people with total responsibility and accountability. This is the opposite of the industry norm, which is full of contracts and theories to shed risk and protect individual interests. You will work with an integrated team of development, design, and construction professionals to transform your vision into reality. Archistruction® is an experience and we want to share it with you.

“It’s not about the building. It’s about what the building enables you to do.” Spend any amount of time with our employees (whom we call “archistructors”) at Neenan, and you’ll hear that phrase come up in conversation.

Discover ideas, engage your community, and improve the learning environment in your schools with creative designs and high-performing spaces.

Whether at the federal, state, or local levels, Neenan ensures that government projects adhere to budgets, reduce waste and construction costs, and emphasize responsible stewardship of tax-payer funds.
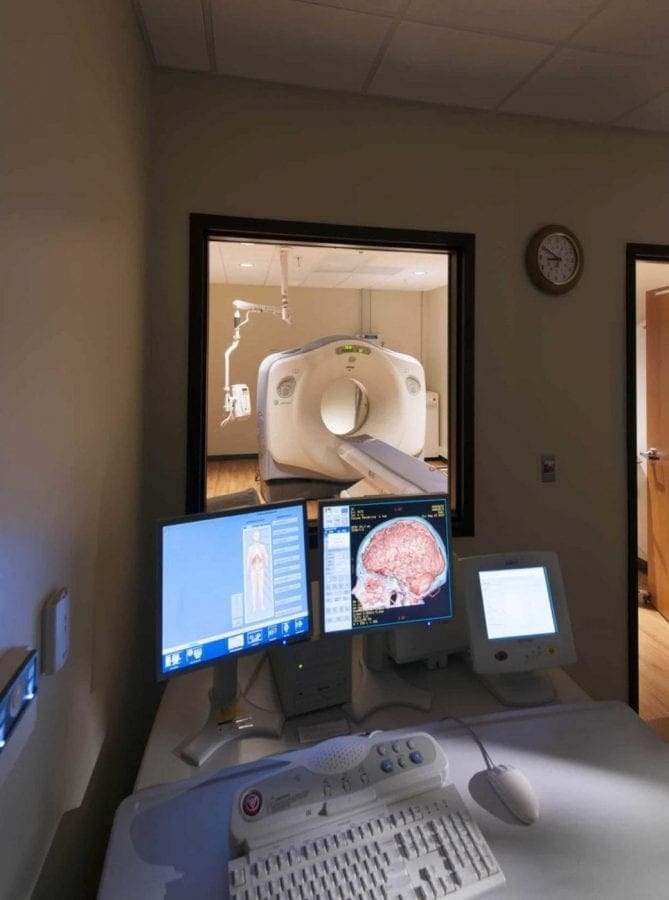
Improve medical care and staff efficiency, optimize your spaces, and attract new patients with community health centers, hospitals, and surgery centers that enhance your healthcare delivery.